Immune Signatures in Early Pregnancy: Predicting Outcomes in ART Patients – Reproduction and Fertility
Reproduction and Fertility shared a post on LinkedIn:
“Day 3 of RaFJC – Immune Signatures in Early Pregnancy: Predicting Outcomes in ART Patients
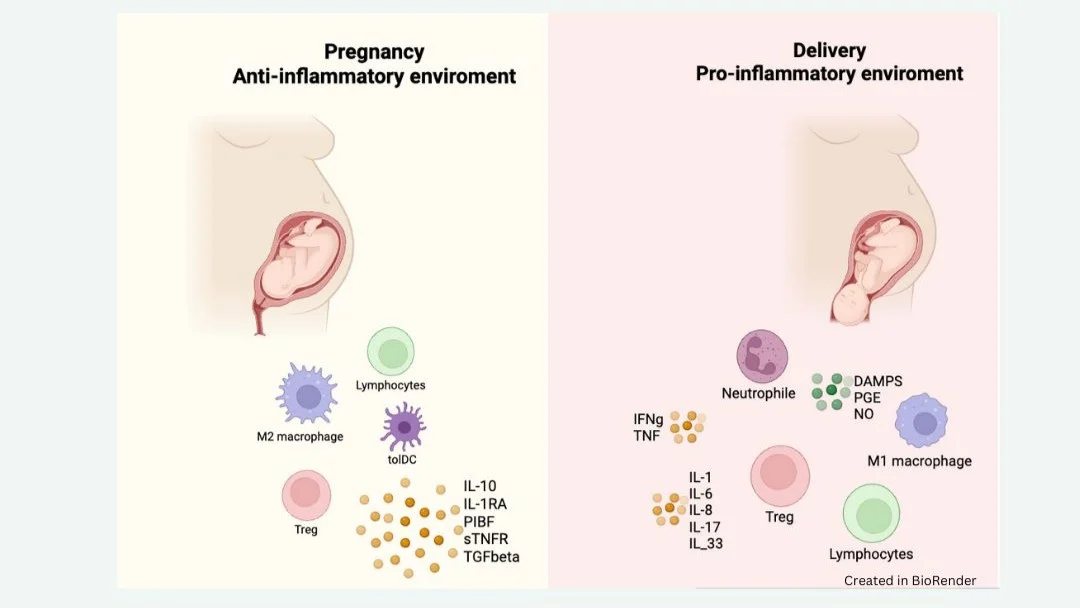
Pregnancy requires a finely tuned immune balance: tolerance of the semi‑allogeneic fetus while maintaining maternal defense against pathogens. Dysregulation of this balance is increasingly recognised as a contributor to implantation failure, recurrent miscarriage, and pregnancy complications.
Recurrent pregnancy loss remains unexplained in up to 40-50% of cases.
Natural killer (NK) cells, T helper subsets, and regulatory T cells (Tregs) are central to maternal immune adaptation.
Identifying early immune markers could allow clinicians to predict pregnancy viability and intervene before complications arise.
Kevin Marron and Conor Harrity performed a prospective pilot study to investigate immune markers in IVF patients at the earliest stage of pregnancy.
Controls:
93 non‑pregnant women analysed in their early follicular phase.
Study group:
65 IVF pregnant women (with unexplained infertility), tested at day 14 post‑frozen embryo transfer after a positive hCG test. The third one of these pregnant women led to a live birth, while 34 ended in miscarriages.
They analysed peripheral blood immunophenotyping by flow cytometry, assessing NK cells, NKT cells, CD4/CD8 T cells, Tregs, and B cells. This design allowed comparison of immune profiles between successful and non‑viable pregnancies at the earliest measurable time point.
This study is the first prospective pilot comparing a comprehensive immunophentyping panel at the exact time of positive hCG, including a differentiation between viable pregnancy and miscarriage cohorts.
What did they find? (image 3)
- B cells (CD19+) and CD57 were increased in all pregnancies, regardless of outcome.
- Treg and CD69 were decreased in pregnancy overall compared to controls (non-pregnant women).
What immune markers were linked to miscarriage? (image 4)
- Reduced pNK CD69+ cells activation during pregnancy, which ended in miscarriage.
- Elevated PNK CD57+ cells during pregnancy, which ended in miscarriage.
Main interpretations?
- A lower pNK activation (CD69) may indicate impaired immune support for implantation and early placentation.
- An elevated pNK CD57+ cells suggest heightened cytotoxic potential, associated with miscarriage risk.
In conclusion
These markers could serve as early warning signals for pregnancies at risk of failure, reducing the need for an invasive biopsy in high-risk patients. Immune profiling at the time of positive hCG could inform early risk assessment in ART patients.”

Stay updated on all scientific advances in the field of fertility with Fertility News.
-
May 1, 2026, 03:13International Expert Recommendations in Emerging Reproductive Science – ESHRE
-
Apr 30, 2026, 18:45AI in Ultrasound Follicular Monitoring Moves Toward Clinical Decision Support – RBMO
-
Apr 30, 2026, 11:42ASRM Encourages Registration for Conference on Practice Growth and Innovation
-
Apr 30, 2026, 11:26ESHRE and ALPHA Launch Global Survey to Update ART Laboratory KPIs
-
Apr 30, 2026, 11:10Susanne Johnson: Advanced Gynaecology Ultrasound Course Day 2
-
Apr 30, 2026, 11:02Platelets Reduce Oxidative Stress Damage in Human Endometrial Stromal Cells in Vitro – RBMO
-
Apr 30, 2026, 10:57GREEG Day 2026: Elevate Your Ultrasound Expertise – GREEG
-
Apr 30, 2026, 10:49Up to Two-Thirds of Elite Female Athletes Experience Irregular Periods – Fertility Plus
-
Apr 30, 2026, 10:47Applications for the ESHRE5 Young Ambassadors 2026 are Still OPEN, But Not for Long! – ESHRE
