
Alisha Tuck: Understanding Endometrial Carcinoma on Ultrasound
Alisha Tuck, OB Gyn, Sonographer at Sonopartners LLC, shared a post on LinkedIn:
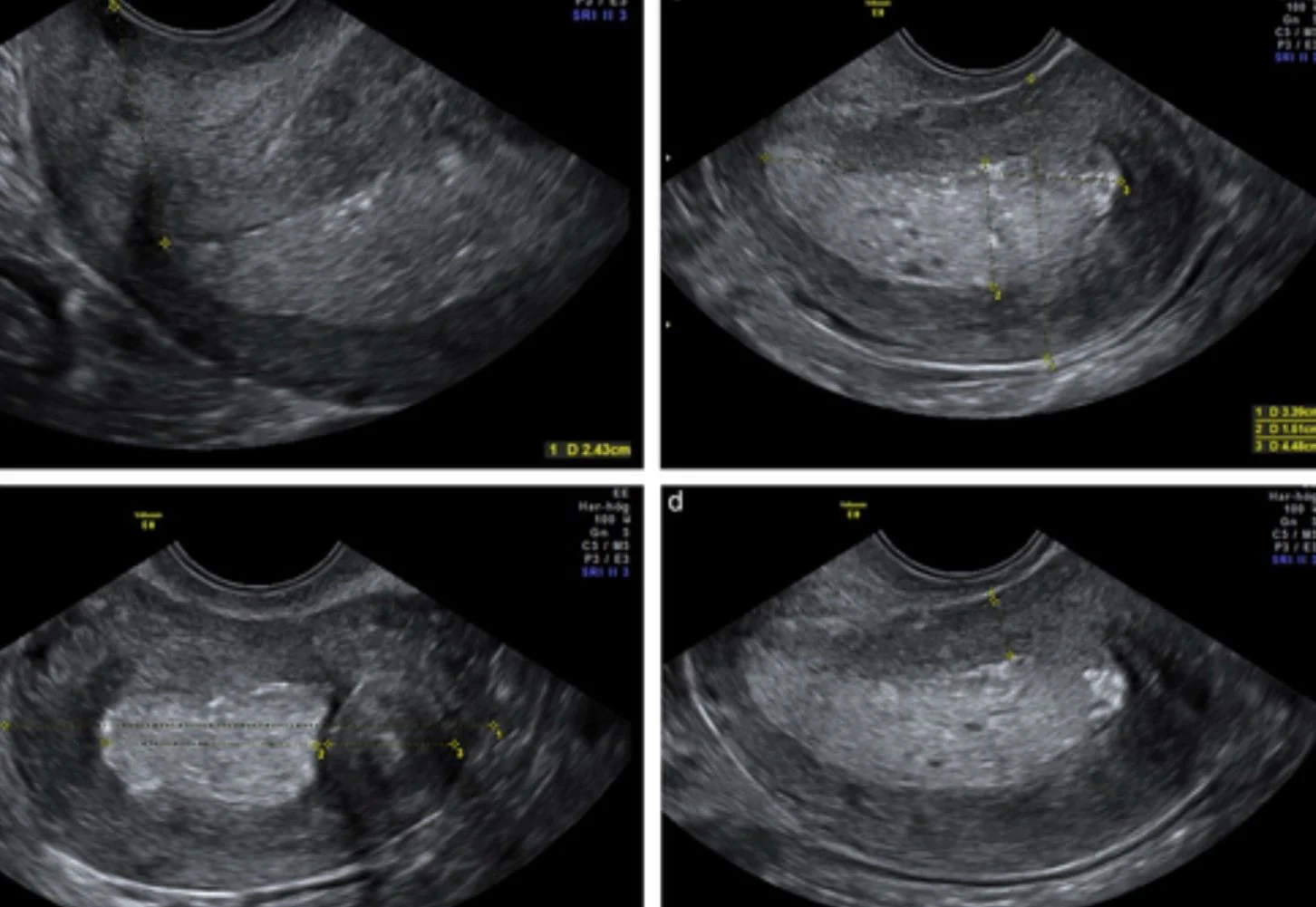
“Understanding Endometrial Carcinoma on Ultrasound
Endometrial carcinoma is the most common gynecologic malignancy in developed countries, primarily affecting postmenopausal women. While a definitive diagnosis requires a tissue biopsy (usually via dilation and curettage or office pipelle), Transvaginal Ultrasound (TVUS) serves as the primary frontline imaging tool for screening and staging.
1. Clinical Presentation and Risk Factors
The hallmark symptom of endometrial cancer is postmenopausal bleeding (PMB). In premenopausal patients, it may manifest as heavy, prolonged, or irregular menstrual cycles.
Key Risk Factors:
- Unopposed Estrogen: Obesity (where peripheral fat converts precursors to estrogen), estrogen-only hormone replacement therapy, or PCOS.
- Tamoxifen Use: Often used for breast cancer treatment, it can have a pro-estrogenic effect on the uterus.
- Lynch Syndrome: A genetic predisposition to various cancers.
2. Sonographic Hallmarks
When evaluating the uterus for malignancy, sonographers and radiologists look for several specific “red flags.”
- Endometrial Thickness (ET): In postmenopausal women with bleeding, an ET > 4 mm is generally considered the threshold for further investigation.
- In asymptomatic postmenopausal women, the threshold is higher (often > 8–11 mm), though this is debated.
- Echogenicity: The endometrium often appears heterogeneous, thickened, and “dirty” or complex compared to the surrounding tissue.
- The Subendometrial Halo: A healthy uterus has a thin, hypoechoic (dark) zone between the endometrium and myocardium. Loss or blurring of this ‘halo’ suggests myometrial invasion.
- Fluid Collections: While simple fluid (hydrometra) can be benign, fluid containing echoes (hemometra or pyometra) in a postmenopausal patient is suspicious.
3. The Role of Doppler Imaging
Color and Power Doppler are essential for differentiating between benign polyps and malignant masses.
- Neovascularization: Malignant tumors often display ‘multiple vessel’ patterns with irregular branching.
- Resistive Index (RI): Malignant flow often exhibits low resistance.
The primary goal of the ultrasound, beyond detection, is to determine how deep the cancer has grown into the uterine wall. This is critical for surgical planning.
Note: MRI is often superior to ultrasound for precise staging (especially for cervical involvement), but TVUS remains the most cost-effective initial assessment.
4. Limitations of Ultrasound
It is important to remember that ultrasound cannot always distinguish between:
- Endometrial Polyps: Often more focal and have a single ‘feeding vessel.’
- Endometrial Hyperplasia: A precursor to cancer that can look identical to early-stage carcinoma.
- Submucosal Fibroids: These can distort the endometrial lining but usually have a distinct, striated appearance.
Disclaimer: For educational purposes only. Correlate with clinical symptoms and histopathological results.”
Stay updated on all scientific advances in the field of fertility with Fertility News.
-
May 14, 2026, 17:13Ribociclib Plus Letrozole in Recurrent Low-Grade Serous Carcinoma of the Ovary – IJGC
-
May 14, 2026, 17:11Christopher Robinson: Isolated Severe Systolic Hypertension During Delivery Admission and Maternal Outcomes
-
May 14, 2026, 17:08Ally Murji: Honoured to Deliver the 51st Annual RT Weaver Lecture at McMaster University
-
May 14, 2026, 17:00Your Hair Dye Could Be Affecting Your Fertility – Fertility Plus
-
May 14, 2026, 16:53Devora Lieberman on Reduced-Tip Needle Design and Its Role in Egg Collection for Older Women – City Fertility
-
May 14, 2026, 16:48AI Can Watch Your IVF Embryo Grow and Predict If It’s Chromosomally Normal, Without Any Biopsy – Fertility Plus
-
May 14, 2026, 12:04Asma Khalil: Why Twin Pregnancies Need More Than Routine Monitoring?
-
May 14, 2026, 12:01Marco Zaccaria: Why Distension Media Selection Matters in Modern Hysteroscopy
-
May 14, 2026, 11:58Mathew Leonardi: PCOS Has Been Renamed to PMOS and It Changes How We Understand the Disease
