
Rukmini Bezbaruah: Interpreting p53 Across Gynaecological Cancers
Rukmini Bezbaruah, Associate Professor Oncopathology at Dr. B. Borooah Cancer Institute, shared a post on LinkedIn:
“Interpreting p53 Across Gynaecological Cancers: One Marker, Multiple Meanings
In gynaecological pathology, TP53 is one of the most frequently altered genes. Yet, its immunohistochemical interpretation is often reduced to a simplistic label – ‘positive’ or ‘negative.’
That approach is no longer acceptable.
p53 must be interpreted as a pattern, and more importantly, in the context of tumour type.
Core principle: Pattern-based interpretation
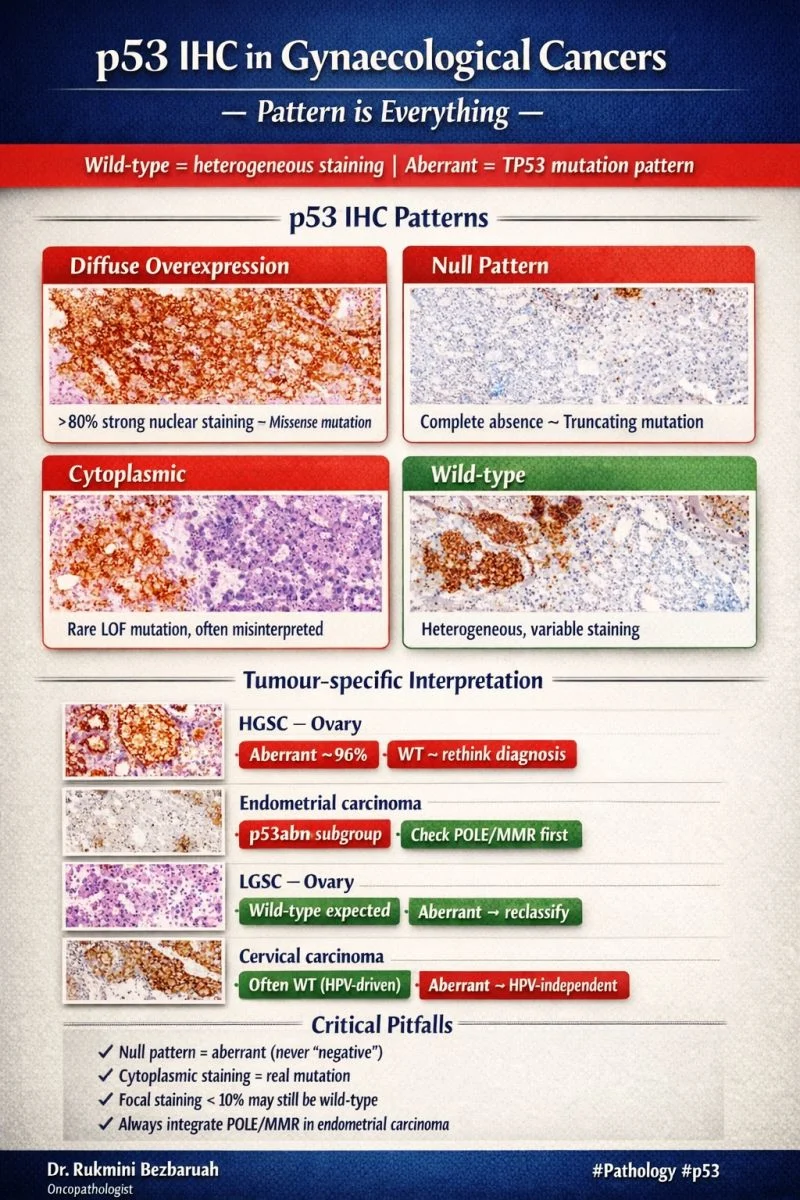
- Wild-type (p53wt) → patchy, variable nuclear staining
- Abnormal (p53abn) →
- Diffuse strong nuclear (overexpression)
- Complete absence (null)
- Cytoplasmic (rare)
- Subclonal (emerging category)
Tumour-specific interpretation matters
1. High-grade serous carcinoma (ovary/fallopian tube)
- Nearly universal p53 abnormality
- p53abn = diagnostic support
- p53wt → reconsider diagnosis
2. Endometrial carcinoma
- Majority are p53 wild-type
- p53abn defines a distinct molecular subgroup with poor prognosis
- Now integrated into molecular classification algorithms
3. Low-grade serous carcinoma
- Typically p53 wild-type
- p53abn → red flag for misclassification
4. Clear cell carcinoma
- Heterogeneous p53 expression
- Interpretation requires strong morphologic correlation
5. Cervical carcinoma
- p53 IHC is less reliable as a surrogate marker
- In HPV-associated tumors, p53 is often degraded → variable staining
What do recent guidelines emphasize?
- p53 is a surrogate for mutation, not a simple marker
- Interpretation must be:
- Pattern-based
- Context-specific
- Integrated with morphology and molecular data
- In endometrial carcinoma, p53 status is now part of:
- ESGO–ESTRO–ESP classification
- FIGO 2023 staging refinement
Common pitfalls
- Reporting ‘p53 positive’
- Missing null pattern due to lack of internal control
- Overcalling wild-type as abnormal
- Ignoring tumour context
Take-home message
p53 does not behave the same across all gynaecological cancers.
Its value lies not just in detection – but in interpretation within the right biological and morphological framework.”
Stay updated on all scientific advances in the field of fertility with Fertility News.
-
May 14, 2026, 17:13Ribociclib Plus Letrozole in Recurrent Low-Grade Serous Carcinoma of the Ovary – IJGC
-
May 14, 2026, 17:11Christopher Robinson: Isolated Severe Systolic Hypertension During Delivery Admission and Maternal Outcomes
-
May 14, 2026, 17:08Ally Murji: Honoured to Deliver the 51st Annual RT Weaver Lecture at McMaster University
-
May 14, 2026, 17:00Your Hair Dye Could Be Affecting Your Fertility – Fertility Plus
-
May 14, 2026, 16:53Devora Lieberman on Reduced-Tip Needle Design and Its Role in Egg Collection for Older Women – City Fertility
-
May 14, 2026, 16:48AI Can Watch Your IVF Embryo Grow and Predict If It’s Chromosomally Normal, Without Any Biopsy – Fertility Plus
-
May 14, 2026, 12:04Asma Khalil: Why Twin Pregnancies Need More Than Routine Monitoring?
-
May 14, 2026, 12:01Marco Zaccaria: Why Distension Media Selection Matters in Modern Hysteroscopy
-
May 14, 2026, 11:58Mathew Leonardi: PCOS Has Been Renamed to PMOS and It Changes How We Understand the Disease
